Physician turnover places a significant strain on healthcare organizations and the broader U.S. healthcare system. It creates several measurable costs, including recruitment expenditures and depressed productivity during new hire ramp-up periods. It also leads to a number of less tangible impacts, such as vacant panels, disrupted referral patterns, and an increased burden on remaining staff.
For healthcare organizations looking to design sustainable and competitive compensation models, protect financial performance, and support long-term growth, understanding the full impact of physician turnover is an essential part of the process.
This article examines the full economic impact of physician turnover and outlines how effective compensation design, administrative support, leadership alignment, and fair market value considerations can aid organizations in reducing turnover risk and protecting long-term performance.
The Economic Burden of Physician Turnover
Physician turnover imposes a substantial economic burden on the U.S. healthcare system, affecting both healthcare organizations and the broader economy. Although the most visible costs relate to recruitment and onboarding, the national financial impact of physician turnover extends far beyond these direct expenses. Lost clinical productivity, disruption of patient access, downstream revenue loss, and increased healthcare utilization all contribute to the overall economic burden.
Research published in the Annals of Internal Medicine estimates that physician burnout costs the U.S. healthcare system approximately $4.6 billion annually, driven by turnover and reductions in clinical work effort. On a per-physician basis, this equates to roughly $7,600 annually per employed physician.1
Primary care illustrates the systemic multiplier effect. Studies estimate that primary care physician turnover generates approximately $979 million in excess healthcare spending annually, with roughly $260 million directly attributable to burnout-related departures. Because primary care physicians anchor referral networks and population health strategies, instability at this level has cascading downstream cost implications across specialty care, emergency utilization, and hospital services.2
At the state level, the economic activity supported by physicians is similarly substantial. States with the largest physician workforces generate hundreds of billions of dollars in healthcare-related economic output annually, as shown in Figure 1 below.3
Figure 1: Estimated Physician-Supported Economic Output by State
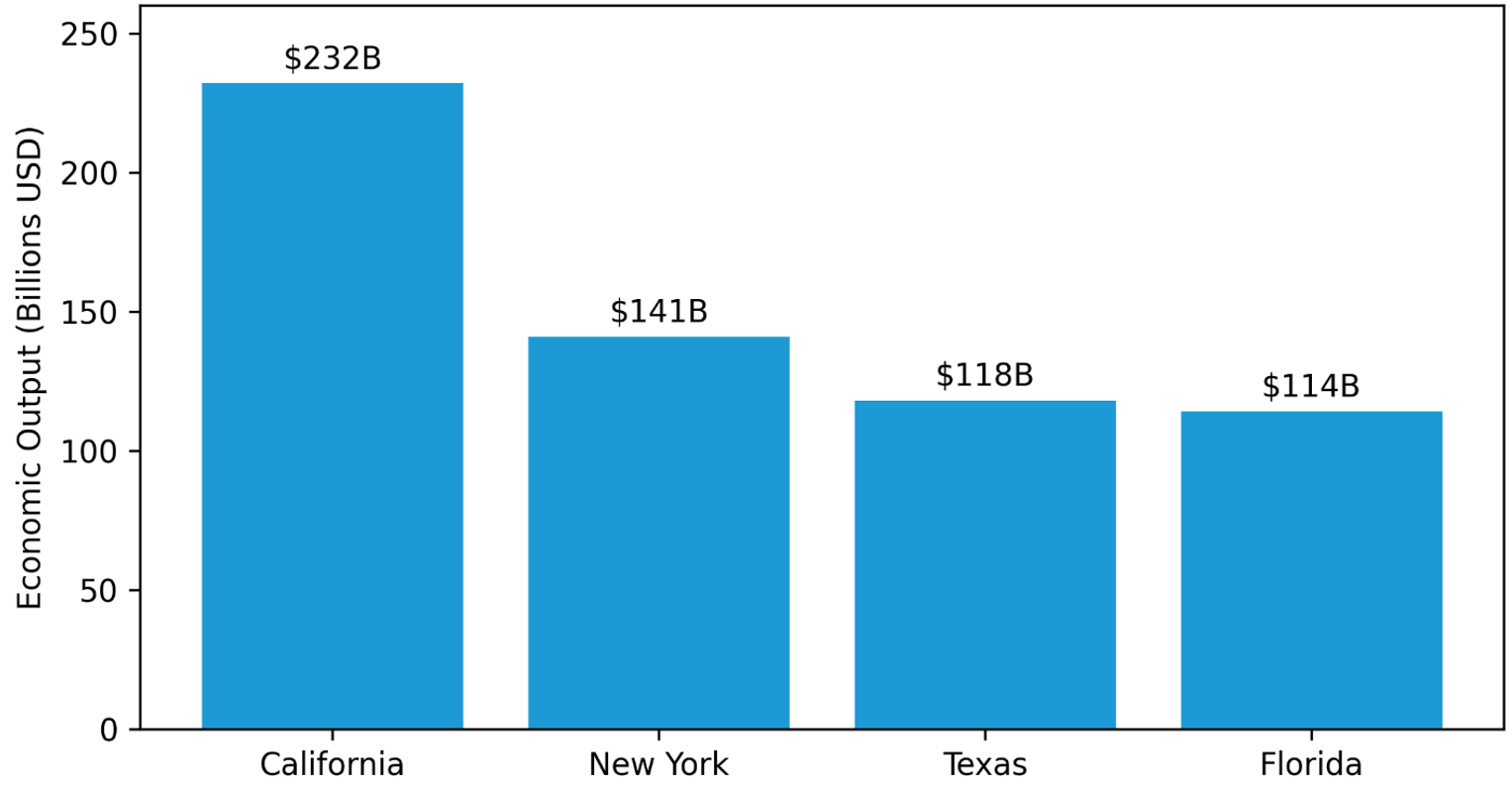
Together, these estimates illustrate how high physician turnover can significantly impact national healthcare expenditures each year. Importantly, these figures are likely to represent only a portion of the total economic burden, as they do not fully capture downstream financial effects on hospitals, health systems, and physician enterprises.
Organizational-Level Financial Exposure
When examining the effects of physician turnover on an organizational level, it is important to consider the direct costs, beginning with recruiting expenditures. Health systems and medical groups typically incur substantial recruitment expenses when replacing physicians, including search firm fees, signing bonuses, relocation packages, and onboarding costs.
A comprehensive review of physician and APP recruiting costs in 2025 published by AMN Healthcare4 reported the following metrics for physicians:
Figure 2: Average Recruiting Expenses per Physician Reported by AMN Healthcare in 2025
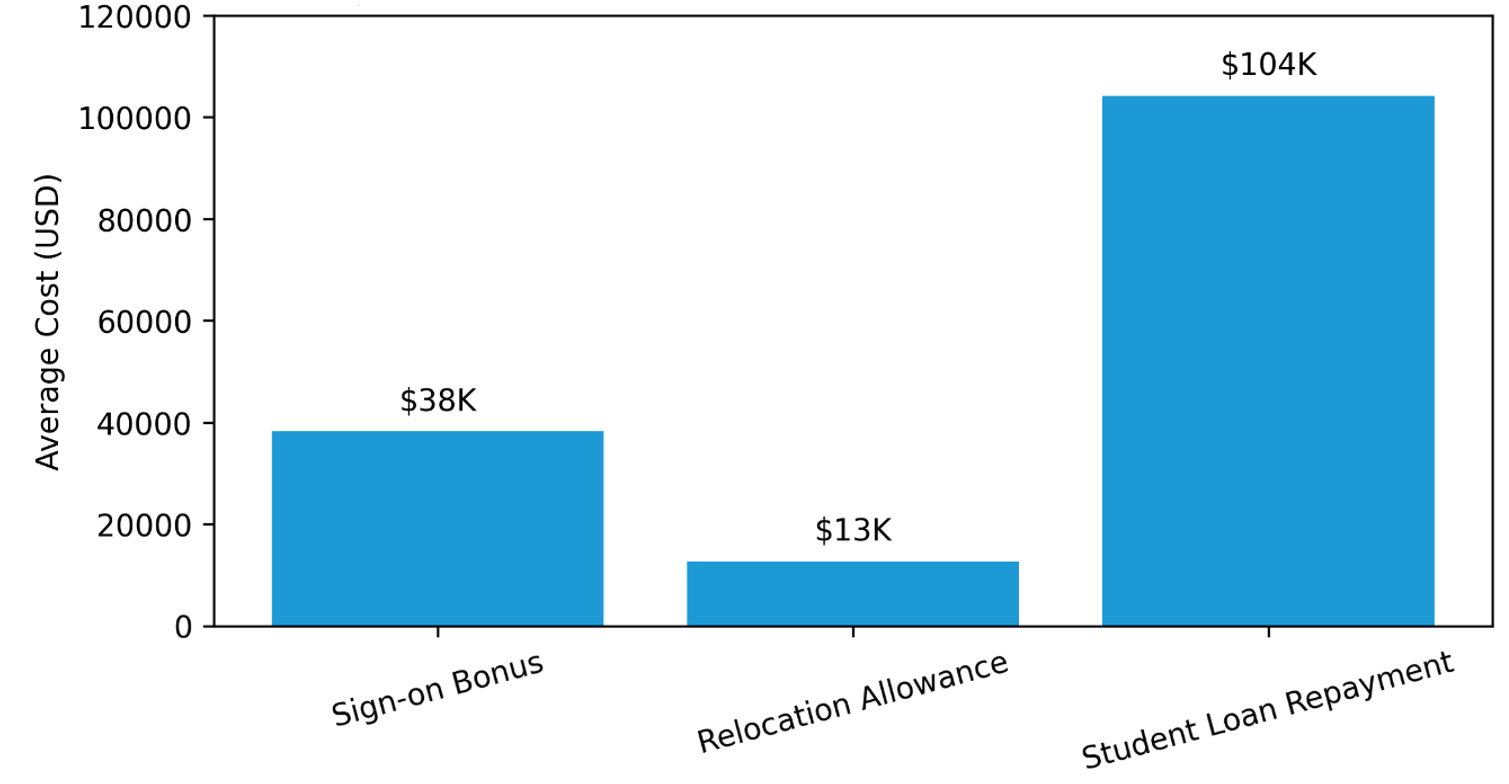
Based on this study, the average estimated cost of recruitment expenditures can total over $150,000 per physician.
Furthermore, industry analyses by AMN Healthcare estimate that the cost of recruiting a replacement physician can exceed $500,000 per hire depending on specialty and market conditions.5
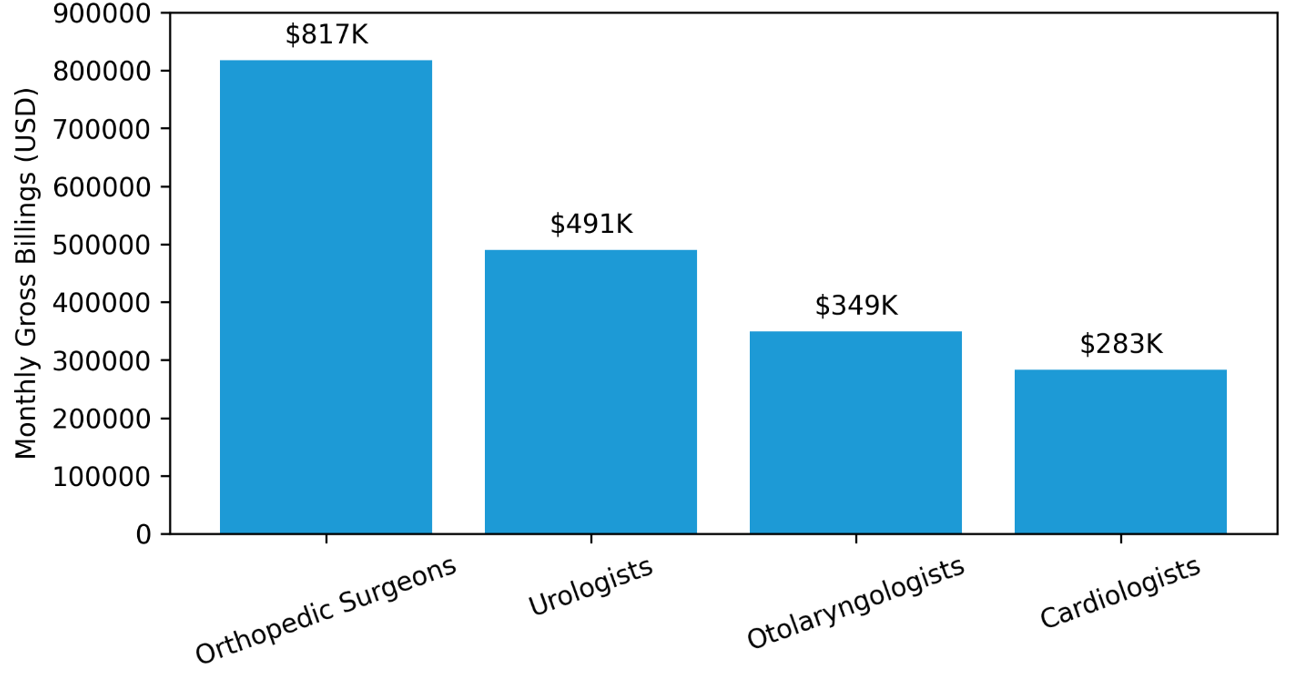
The direct cost of physician turnover is two-fold: costs are incurred to replace the provider in addition to the lost revenue due to the vacancy. High-demand specialties can generate hundreds of thousands of dollars in monthly billings. Data from national physician workforce reports indicate that the estimated monthly gross billings associated with vacant physician positions may range anywhere between $300,000 and $800,000 depending on the specialty, further outlined in Figure 3 below.
Figure 3: Estimated Monthly Revenue Loss From Vacant Physician Positions
Secondary and Downstream Financial Effects
As positions remain vacant, health systems are faced with a disruption of referral patterns and decreased volume stability. Even when the positions are filled, it takes a significant amount of time to stabilize these patterns and establish continuity.
Devoting time, money, and energy to replacing providers has another secondary effect: increased strain on remaining staff. These providers experience a general decrease in morale and potential increase in worked hours and administrative burden, all leading to a heightened risk of physician burnout. Healthcare organizations may look to hire part-time or locum tenens providers to fill coverage gaps temporarily. More often than not, hourly rates for these providers include a markup. Additionally, in rural markets, hospitals incur costs associated with reimbursing locum tenens physicians for travel, lodging, and meals.
Lastly, compensation models often take into consideration certain quality standards that must be met in order to receive a portion of the physician’s base compensation or additional quality bonuses. The quality metrics can include abiding by predetermined response times, meeting patient satisfaction or access goals, and complying with documentation standards. Physician turnover can make it increasingly difficult to achieve departmental goals as positions remain vacant, while the remaining staff is faced with increased strain and burnout.
Burnout as a Precursor to Turnover Risk
Burnout remains one of the strongest predictors of physician intent to leave. Emotional exhaustion, depersonalization, and reduced professional fulfillment correlate directly with increased turnover probability and reduced clinical full-time equivalent (FTE) effort. Importantly, burnout can erode productivity well before a formal departure. Reduced clinical hours, decreased engagement, and increased administrative inefficiency impose measurable opportunity costs. For a 500-physician enterprise, even the estimated $7,600 annual burnout-related cost per physician represents nearly $4 million in annual exposure. Addressing burnout, therefore, should be viewed not only as a wellness initiative but as a financial risk mitigation strategy.
Strategic Implications for Healthcare Leaders
The economic effects of turnover (lost contribution margin, recruitment expense, and service line disruption) underscore the need for deliberate strategies that address both physician engagement and structural alignment. While no single intervention eliminates turnover risk, organizations that approach physician retention through a coordinated strategy such as integrating compensation design, operational support, and leadership alignment are better positioned to stabilize their workforce and protect long-term financial performance.
Aligning Compensation With Sustainable Workload Expectations
Compensation design is one of the most influential drivers of physician retention. In hospital-employed models, compensation plans frequently rely on productivity benchmarks, such as work relative value units (wRVUs), combined with quality or citizenship components. When these benchmarks are not aligned with operational realities (e.g., patient complexity, staffing shortages, or administrative burden), physicians may experience pressure to maintain productivity levels that are not sustainable long term.
Health systems can mitigate this risk by:
- Establishing transparent productivity benchmarks based on reliable market data
- Incorporating balanced incentive structures that reward quality, patient access, and team-based care
- Periodically reassessing compensation models to ensure continued alignment with clinical workflow and system priorities
For example, some compensation plans include tiered productivity thresholds or incentive pools that recognize variations in patient panel size, complexity, or procedural mix. Others have integrated group-based productivity metrics to reduce pressure on individual physicians while encouraging collaborative care models across a practice.
Reducing Administrative Burden and Improving Practice Infrastructure
Administrative inefficiencies are consistently cited as a major contributor to physician burnout. Excessive documentation requirements, inefficient electronic health record (EHR) workflows, and inadequate staffing support can significantly reduce clinical efficiency and professional satisfaction.
Health systems can address these issues through targeted operational investments, such as:
- Expanding clinical support staff
- Optimizing EHR workflows to reduce documentation time
- Implementing centralized prior authorization or referral management teams
- Leveraging technology to streamline patient communication and scheduling
Strengthening Physician Leadership and Governance
Physician engagement often improves when clinicians have meaningful input into operational and strategic decisions. Health systems that incorporate physicians into leadership roles within the system, such as service line leadership, may experience stronger alignment between administrative priorities and clinical realities.
Leadership development programs for physicians can also enhance retention by creating professional growth pathways and fostering stronger collaboration between physicians and health system executives. By investing in physician governance structures, organizations can better identify emerging workforce challenges and address concerns before turnover happens.
Addressing Burnout Through Workforce Design
Workforce design strategies represent another important lever for physician retention. Examples include:
- Flexible scheduling models or part-time employment options
- Panel management and care team expansion in primary care
- Adequate call coverage and workload distribution
While these initiatives may require incremental investment, they can generate meaningful financial returns if they reduce turnover rates or prevent productivity declines associated with burnout.
The Role of Valuation and Fair Market Value Considerations
As health systems pursue retention strategies, compensation design must remain compliant with regulatory and valuation standards. Physician compensation arrangements should adhere to fair market value (FMV) and commercial reasonableness requirements under federal healthcare regulations, such as the Stark Law and Anti-Kickback Statute.
Valuation analysis plays an important role in helping organizations balance two competing priorities: offering competitive compensation necessary to recruit and retain physicians while ensuring that compensation structures remain defensible from a regulatory standpoint.
Independent valuation assessments can help organizations:
- Benchmark physician compensation against relevant market data
- Evaluate the financial sustainability of compensation models
- Assess whether compensation arrangements remain commercially reasonable given the health system’s strategic objectives
- Document the rationale supporting compensation decisions
This process becomes particularly important when addressing physician shortages. Health systems may face pressure to increase compensation levels to recruit or retain physicians, especially in high-demand specialties or difficult to recruit locations. A thoughtful valuation process allows organizations to evaluate whether such adjustments remain consistent with FMV and aligned with the organization’s broader financial strategy.
Competitive Compensation as a Retention Strategy
Competitive compensation alone does not guarantee retention, but it remains a foundational element of physician engagement. Physicians are increasingly comparing employment opportunities across health systems, independent practices, and emerging care delivery models. Compensation structures that are perceived as inequitable or misaligned with workload expectations can accelerate turnover.
Effective compensation plans typically share several characteristics:
- Transparency in productivity expectations and incentive calculations
- Alignment between compensation and organizational goals, such as access or quality outcomes
- Flexibility to adapt to evolving clinical and market conditions
- Clear communication regarding how compensation compares to relevant market benchmarks
When supported by sound valuation analysis and thoughtful governance, competitive compensation models can serve as a stabilizing force within hospital-employed physician medical groups.
Conclusion
Physician turnover carries costs that extend far beyond recruitment expense. It disrupts revenue continuity, compresses margins, destabilizes care delivery, and introduces strategic uncertainty. In an environment defined by workforce shortages and economic pressure, retention is increasingly a financial strategy.
As national physician shortages intensify and healthcare organizations continue to operate under increasing financial pressure, the ability to quantify, manage, and mitigate physician turnover will remain a critical competency for healthcare leaders. Organizations that approach physician workforce stability with the same rigor applied to other strategic investments will ultimately be better equipped to protect both mission and margin in an increasingly complex healthcare environment.
- Han S, Shanafelt TD, Sinsky CA, et al. Estimating the attributable cost of physician burnout in the United States. Ann Intern Med. 2019;170(11):784-790. doi:10.7326/M18-1422.
- Sinsky CA, Shanafelt TD, Dyrbye LN, Sabety AH, Carlasare LE, West CP. Health care expenditures attributable to primary care physician overall and burnout-related turnover: a cross-sectional analysis. Mayo Clin Proc. 2022;97(4):693-702. doi:10.1016/j.mayocp.2021.09.013.
- American Medical Association. The economic impact of physicians in the United States. AMA; 2023. Accessed March 11, 2026. https://www.ama-assn.org/press-center/press-releases/physicians-support-126-million-jobs-and-23-trillion-economic-output
- AMN Healthcare. 2025 Review of Physician and Advanced Practitioner Recruiting Incentives. AMN; 2025. Published 2025.
- AMN Healthcare. The Cost of Physician Turnover and the Economic Impact of Physicians. AMN Healthcare White Paper. Published 2023.